Unraveling the Mystery: How Genetics Influence Asymptomatic COVID-19
Latest Research ties link with common HLA Class I variant, HLA-B*15:01
Dear Readers,
Welcome to Science Simplified, a newsletter which Unlocks the Wonders of Science, One Simplified Concept at a Time!
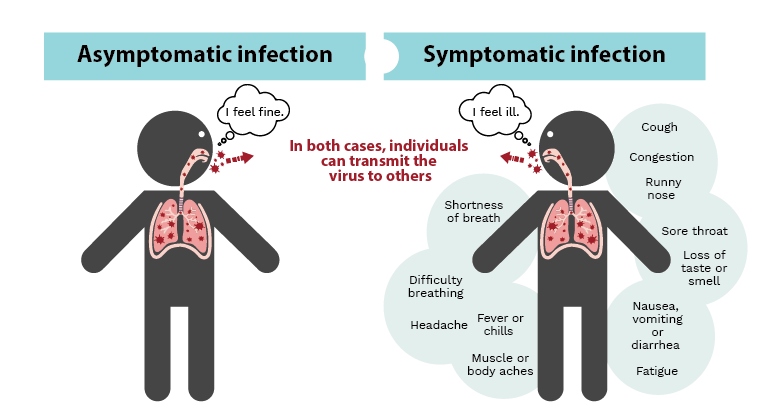
In this edition, we will delve into the science behind asymptomatic COVID-19 infections. Asymptomatic infections refers to a situation where a person contracts SARS-CoV-2 virus, responsible for COVID-19, but doesn't exhibit noticeable symptoms - no cough, no fever, no trouble breathing. These carriers, though symptom-free, can still spread the infection. While asymptomatic cases are not exclusive to SARS-CoV-2, they have gained significant attention during the pandemic due to their high prevalence. This has posed challenges for public health efforts to track and control the virus's spread, describes as “Achilles heel” of the pandemic.
Until now, much of the scientific focus has centered on severe cases of COVID-19. However, asymptomatic infections offer a unique opportunity to study how the immune system can swiftly clear the virus without causing illness. Insights gained from these 'COVID-19 virgins' can pave the way for improved therapies in the face of future coronavirus outbreaks.
This mystery has recently been unraveled. Scientists have pinpointed a genetic factor linked to a higher likelihood of remaining symptom-free after a SARS-CoV-2 infection. In this article, we will break down this groundbreaking discovery and elucidate the fundamental science behind how the immune system identifies viral infections.
Science Simplified, is a reader-supported publication that covers diverse topics directly impacting your lives. To receive new posts and support my work, consider becoming a free or paid subscriber.
Asymptomatic Infections: No symptoms but Infectious!
Have you had COVID-19 without showing symptoms? or Do you know someone in this situation, or someone who claims they never got infected, even when their partner was sick in bed?
This is the case of Asymptomatic COVID-19 infections, which refer to cases in which individuals are infected with the SARS-CoV-2 virus but do not develop any noticeable symptoms.
Silent Spreaders of COVID-19
Asymptomatic individuals didn’t felt sick so they were unknowingly spreading the virus to others. Studies have shown that asymptomatic individuals can have viral loads (the amount of virus in the body) similar to or even higher than those with symptoms. They can exhale respiratory droplets containing the virus, which can potentially infect others. Henceforth, they were referred to as the “silent spreaders” and estimated to account for over 20% of all COVID-19 infections.
During pandemic, we all witnessed how these silent spreaders posed a great challenge to control the spread of covid-19 virus. However, we didn't know precisely why, even after getting infected, these individuals didn't feel sick or exhibit any symptoms. These asymptomatic cases didn’t had any antibodies to coronavirus (SARS-CoV-2), meaning they somehow avoided catching it.
What is it that clears the virus before it gets a foothold?
Either these individuals are protected from contracting the virus or neutralise it before it could make them sick. What’s the mystery? Can we learn from these cases to protect symptomatic individuals?
Now, scientists have solved this mystery. A research study published in Nature on July 19 highlights the role of genetics in providing protection against SARS-CoV-2.
Let’s explore!!
Asymptomatic cases possessed pre-existing immunity against SARS-CoV-2
In a recent study, scientists found that asymptomatic individuals were naturally endowed with a genetic defense against SARS-CoV-2. This defense stemmed from the presence of HLA-B*15:01, a specific variant of the HLA gene. Put plainly, this variant facilitated immune cells in recognizing and neutralizing the virus before it could cause illness. Essentially, these individuals had a built-in immunity to SARS-CoV-2, thanks to their genetics, granting them pre-existing T cell protection.
This is a surprise! Prior to this recent study findings, it was understood that, any natural born immunity was unlikely.
In nature, it appears that Genetics-based Protection Against Infections is a rare phenomenon. AIDS remains one of the few viral diseases where a mutation in a person’s gene can protect them from AIDS. Similarly, some individuals genetics protect them from conditions like Malaria and Norovirus. On the other hand, there are ample instances where genetic mutation has shown to increase the susceptibility to noncommunicable diseases such as sickle cell anaemia, cystic fibrosis and various cancers.
Before going any further, let’s understand the role of HLA.
HLA, also known as human leucocyte antigen are like nametags on the surface of our cells. They help our immune system recognize which cells belong to our body and which might be from a foreign invader like a virus or bacteria, basically acting like an overzealous guard dog.
There are thousands of different types of HLA, which can be mainly classified into two major groups: HLA Class I and HLA Class II.
HLA Class I:
HLA-A, HLA-B and HLA-C are the three main genes in this class.
They are found on all cells in the body.
They play a crucial role in informing the immune cell about a viral attack by presenting pieces of viral or abnormal proteins (antigens) to the immune cells.
HLA Class II:
HLA-DR, HLA-DP and HLA-DQ are the main genes in this class.
These genes are majorly found on specialised immune cells like B cells, macrophages (big cell eaters) and dendritic cells.
These HLA Class II genes on specialised immune cells play important role in presenting antigens from pathogens (like bacteria) to other immune cells (like helper T cells), which then coordinate the immune response.
In essence, these thousands of HLAs play a significant role in helping our defence army (immune system) to distinguish between “self” (the body’s own cells) and “non-self” (foreign substances like viruses or bacteria). They act as messengers, alerting our immune system to potential threats such as invasion by foreign elements like bacteria, viruses or protozoans, etc.

Each HLA variant can have slightly different properties in terms of which antigens (pieces of viral proteins) they can present. When it comes to our immune responses, HLA variants play a major role in how our bodies handle viral infections. They can either influence susceptibility or resistance to certain diseases.
In short, HLA variants have a big impact on how we deal with infections.
HLA-B*15:01
It is a variant of HLA-B gene. Like other HLA variants, it plays a role in presenting antigens (pieces of viral proteins) to T cells, which are a crucial part of the immune response. This presentation helps the immune system recognize and respond to the virus.
Prior to understanding its role in recognising SARS-CoV-2, it was observed that individuals with the HLA-B*15:01 variant were at increased risk of developing a severe allergic reaction to Abacavir, a drug used in the treatment of HIV.
Robust Immune Response in HLA-B*15:01 Carriers
Jill Hollenbach, an immunologist at the University of California, San Francisco led the study with her team, they discovered the role of HLA-B*15:01 in recognising SARS-CoV-2 and alerting the immune cells to attack and neutralise the virus in body. They followed about 30,000 people registered in National Donor Program (which includes roughly 13 million people — all with neatly logged HLA types) from the beginning of the pandemic until April 2021, when the vaccines became widely available.
Out of 30,000 people included in the study, more than 13,000 ultimately tested positive for COVID-19. About ten percent (1,428 individuals) of COVID-19 positive cases were totally asymptomatic, no symptoms, not even scratchy throat. For all study participants, they performed high-resolution genotyping for five highly abundant and variable HLA class I and Class II genes. They found that Class I HLA version, HLA-B*15:01 was significantly overrepresented in asymptomatic group relative to symptomatic individuals. Their findings also showed that one copy of this gene variant was linked to twice as likely to have no symptoms with COVID-19 infection. That protection increased by more than eight times if a person had two copies of the gene.
"To be fair, not everybody that has [HLA-B*15:01] will be asymptomatic," Hollenbach says. "But it was a really clear, robust and replicable association." Hollenbach also pointed out that, "The genetic association that we found in this study explains some but not all asymptomatic disease."
Furthermore, this study examined the structure of HLA-B*15:01 molecule alongside specific antigen peptides (small fragments of protein) from SARS-CoV-2 and some common seasonal coronaviruses. They found out that this HLA variant can flag both spike peptides and peptides from other seasonal coronaviruses to immune cells, which in turn activates the immune cascade to neutralise virus.
This clearly indicates pre-existing T cell immunity against SARS-CoV-2 in a subset of individuals carrying HLA-B*15:01 who did not have any previous contact with SARS-CoV-2. Additionally, individuals carrying this HLA variant also show cross-reactive immunity against common seasonal coronavirus strains (seasonal cold viruses).
HLA-B*15:01 Enables Swift Viral Clearance at Entry Point
Several studies demonstrated that T cells (immune cells) in asymptomatic SARS-CoV-2 cases respond strongly, much like in symptomatic cases. Recent research has found that memory T cells targeting SARS-CoV-2 virus are more concentrated at the site of infection. This suggests that pre-existing memory T cells at the entry points for the virus may lead to a swift elimination of the virus before symptoms appear.
Memory T cells are a type of specialized immune cell that have a remarkable ability to "remember" specific pathogens, like viruses or bacteria, that they have encountered in the past. Once they've dealt with a particular germ, they retain a memory of it. If that same germ tries to invade the body again, these memory T cells can quickly recognize it and mount a swift and targeted immune response. They play a crucial role in providing long-lasting immunity against previously encountered infections. This is similar to how many vaccines, including the COVID vaccine, work.
When individuals with HLA-B*15:01 encounter a common cold virus, their immune system generates Memory T cells that closely resemble those needed to combat COVID-19. This "template" provides a level of defense against the virus, potentially allowing them to remain symptom-free even if infected. Additionally, in asymptomatic cases, T cells release more IFNγ early in the infection compared to symptomatic cases, indicating a significant role for memory T cells at this stage.
Besides, it has been suggested that these asymptomatic individuals may develop a robust immune responses that will prevent them from future infections. Future research will further ascertain this notion.
Conclusion
This study provides strong evidence that a common genetic variation in a specific immune system component, known as HLA-B*15:01, is closely linked with asymptomatic COVID-19 cases. People with this genetic variant already had a type of immune system defense, called T cell immunity, against SARS-CoV-2. This immunity likely developed from past encounters with other similar coronaviruses that cause common seasonal illnesses.
This study sheds light on why certain individuals remain symptom-free despite being infected with COVID-19. While the genetic link uncovered here accounts for some cases of asymptomatic disease, it represents just the beginning of our understanding. Research like this paves the way for improved treatments in future infections.



