The Future is Here: The Pill That Promises to Trim Fat like Never Before
Groundbreaking Leap in Obesity Medicine
Dear Readers,
Welcome to Science Simplified, a newsletter which Unlocks the Wonders of Science, One Simplified Concept at a Time!
In this edition, we delve into the remarkable advances in Obesity Medicine, where scientists have made groundbreaking strides in understanding and suppressing hunger. In this article, you will learn about the following:
Obesity: When fat gets in the way of health
Ways to measure obesity at home and clinical screening methods
Why we should pay attention to abdominal obesity
Obesity prevention: It's not always about willpower
Biological basis of Appetite Regulation: Role of hunger and satiety hormone
The promising role of anti-diabetic drugs in weight-loss
A leap forward in Obesity Medicine: Examining the past, present, and future
Resetting expectations: Promising outcomes in weight-loss treatment
Concluding Remarks: Emphasizing the significance of a balanced approach to health

We hope this edition provides you with valuable insights and inspires you to stay informed about the latest advancements in Obesity Medicine.
Thank you for subscribing to Science Simplified. Kindly consider upgrading to a paid subscription to support our newsletter. By doing so, not only will you gain access to additional benefits, but you will also contribute to the continued production of informative content that can make a positive impact on the lives of our readers.
Obesity: When Fat gets in the way of Health
Obesity is the excess or abnormal accumulation of fat in body to an extent that it may have a negative impact on health.
When your Body-Mass-Index [BMI = weight (in kilograms) / (height (in meters))^2] is above 30, you are classified as Obese. Another way of knowing whether you are in obese category, is by measuring Waist to Hip Ratio (WHR), this gives an estimate of abdominal obesity. Males above 0.90 WHR and females above 0.85 WHR will be clinically obese. BMI and WHR are simple and widely used screening tools, but they ignore individuals’ bone density, fat distribution, muscle mass. Henceforth, to measure body composition accurately, you might need DEXA Scan, BIA, DXA scans. These scans can reliably inform you about bone density, muscle mass and fat mass distribution in the body.
Obesity is a medical condition, sometimes considered a disease as it often comes with heightened risk of metabolic disorders such as type 2 diabetes (T2D), heart diseases, sleep apnea, and certain cancers (including endometrial, breast, ovarian, prostate, liver, gallbladder, kidney, and colon).
Obesity is growing exponentially, it has nearly tripled since 1975. According to World health Organisation (WHO), in 2016, worldwide about 40% of adults were overweight and 13% had obesity. According to World Obesity Federation, the number of people with obesity has increased to 764 million in 2020.
Obesity can result from a combination of various factors, including genetic predisposition, environmental influence, dietary habits (like high-fat, high-sugar, high-salt, energy-dense, and micronutrient-poor foods), physical activity levels, underlying medical conditions and societal changes, etc.
Obesity is Preventable
Yes, obesity can be reversed. How ? Follow the First Law of thermodynamics: Law of Energy Conservation! This law states that energy cannot be created or destroyed; it can only be transferred or transformed from one form to another. In the context of weight loss, increase your energy expenditure and decrease your energy intake to reduce weight. This is just fancy way of saying Eat Less and Exercise More!

This is the universal recommendation for weight loss but unfortunately this formula dose’t work for everyone. For some initial results of dieting+exercise are promising which plateaus in the long term, leading to return to old eating habits and subsequent weight gain. Then there are others who don’t seem to get any benefit from dieting. By acknowledging the limitations of a universal weight loss formula and considering the complexities of individual experiences, we can shift the focus from solely attributing weight loss success or failure to willpower.
Bariatric Surgery: When traditional ‘Eat Less’ approach Fails
Bariatric surgery is typically recommended for obese individuals with significant obesity-related health complications who have not achieved sustainable weight loss through non-surgical methods as discussed above. It involves altering the digestive system to restrict food intake, decrease nutrient absorption, or a combination of both. The two most common types of bariatric surgery are gastric bypass and sleeve gastrectomy. Such surgeries results in significant and sustained weight loss, leading to improvements in obesity-related health conditions such as type 2 diabetes, high blood pressure, sleep apnea, and joint pain. It can also improve overall quality of life, self-esteem, and psychological well-being.
However, it is not a one-size-fits-all solution, there is considerable variations in the outcomes and the benefits across time in some patients.
Obesity Medicine: Past, Present and Future
As scientific understanding progresses, new insights emerge. The field of obesity medicine has witnessed significant advancements over the years, transforming the way we approach weight loss.
Similarly, over the years, views regarding being overweight have undergone drastic changes. There was a time when certain cultures viewed obesity positively, associating it with wealth and fertility. However, this perception shifted in 2013 when several medical societies, such as the American Medical Association and the American Heart Association, officially recognized obesity as a disease.
Here, we will explore the advancements in obesity medicine by delving into the past, present, and what lies ahead in the future.
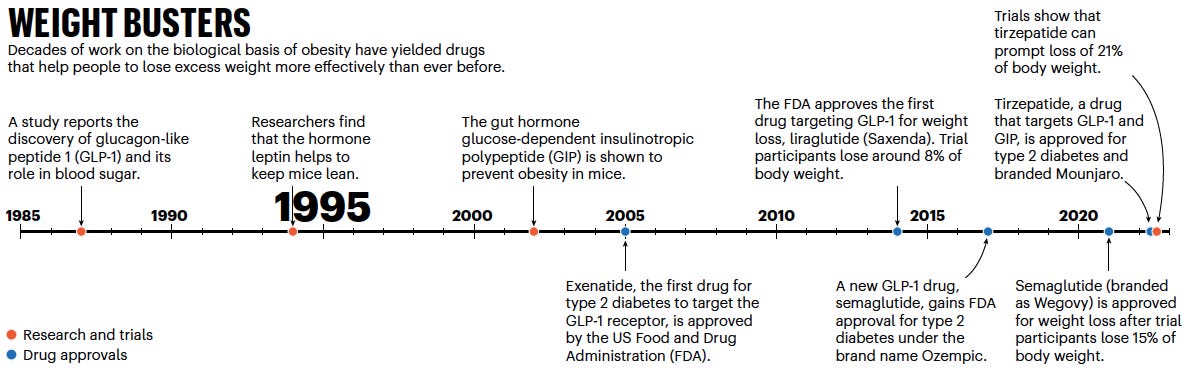
Past
In 1994, Jeffery Friedman's discovery of a faulty gene related to the hormone Leptin transformed our understanding of the biological roots of obesity and appetite regulation. This breakthrough sparked a surge of research into pharmacological treatments.
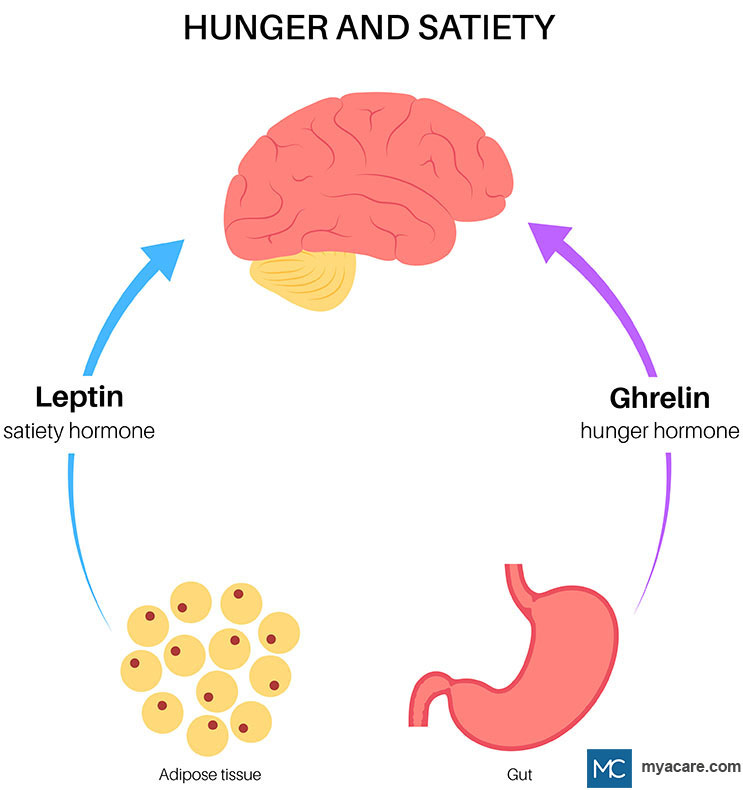
Little background on Leptin: Leptin is hormone which is produced by fat cells, it acts as a long-term regulator of energy balance and body weight. It helps regulate food intake and energy expenditure by signaling to the brain about the body's energy stores. Leptin is commonly known as ‘satiety hormone’ or ‘fat hormone’. The primary function of leptin is to signal the brain when we have enough energy stored in our body fat and to suppress appetite. When fat cells release leptin into the bloodstream, it travels to the brain and acts on receptors in the hypothalamus, promoting feelings of fullness and reducing appetite. This helps to maintain a stable body weight by regulating food intake and energy expenditure.
In individuals with obesity, a person may have high levels of leptin circulating in their bloodstream. However, their brain may become resistant to the effects of leptin, resulting in a diminished response to its appetite-suppressing signals. This condition is known as leptin resistance, which can contribute to continued overeating and weight gain.
Appetite regulation is a complex process involving multiple factors, accompanying Leptin in this role is Ghrelin
Little background on Ghrelin: It is a hormone discovered in 1999, it was initially identified for its ability to stimulate the release of growth hormone from pituitary gland. However, it was later recognised that ghrelin also has potent effects on appetite and energy balance.
Ghrelin is predominantly produced in the stomach and stimulates appetite. It signals hunger to the brain and increases food intake. Ghrelin levels go up before meals and go down after we eat. When our stomach is empty or when we're on a calorie-restricted diet, ghrelin levels tend to increase, signaling to the brain that we need to eat. This increase in ghrelin triggers sensations of hunger and motivates us to search for food. On the other hand, when we eat and our stomach is stretched, ghrelin levels decrease, leading to a decrease in hunger. It also affects other parts of our brain that are involved in pleasure and motivation related to food. Ghrelin is commonly known as ‘hunger hormone’.
It is higher in people with obesity, and problems with ghrelin can contribute to difficulties in controlling appetite and gaining weight. This might seem counterintuitive since higher ghrelin levels are typically associated with increased hunger. However, it's believed that in cases of obesity, the body's response to ghrelin may be altered, leading to a reduced sensitivity to its appetite-suppressing effects. This can contribute to overeating and difficulties in weight management.
While Leptin therapy has shown promise in treating rare cases of genetic leptin deficiency, its effectiveness in treating common obesity is limited. Leptin therapy has not received FDA approval for non-genetic cases due to modest weight loss and serious side effects, especially cardiac risks.
Present: Obesity drugs that Quash Hunger
Type-2 Diabetes Drug with promising Weight-Loss Effect
In 1987, Glucagon-like peptide (GLP-1) was discovered and soon became popular for its role in regulating blood glucose levels by stimulating insulin and suppressing glucagon. In 2015, the first GLP-1R agonist (brand name: exenatide) was approved by the US Food and Drug Administration (FDA) for the treatment of T2D, which was followed by other GLP-1R agonists approved in 2010 (liraglutide), 2014 (dulaglutide), 2016 (lixisenatide), 2017 (semaglutide, subcutaneous) and 2019 (semaglutide, oral).
Interestingly, in two different clinical trial of liraglutide, T2D participants on these drugs also lost weight, which was a welcome positive side-effect of the drug. Studies further revealed the role of GLP-1 in appetite regulation.
How GLP-1 leads to weight-loss:
Increased satiety: GLP-1 binds to GLP-1 receptors in the brain, specially in the hypothalamus, which is involved in appetite regulation. By binding, receptor is activated and feeling of fulness and satiety is increased, leading to increased feelings of fullness and reduced appetite.
Slowed gastric emptying: GLP-1 also delays the emptying of food from the stomach into the intestines. This delay results in prolonged digestion and absorption of nutrients, leading to increased feelings of fullness and reduced appetite.
Decreased food cravings: GLP-1 activates the brain centers involved in reward and food-seeking behaviors.
Increased energy expenditure: GLP-1 increases energy expenditure (calorie burning) in the body. This effect is partly due to their action on brown adipose tissue, which is involved in thermogenesis (heat production) and energy expenditure.
Liraglutide has shown the ability to induce an average weight loss of about 8%, which is 5 percentage points higher than those taking a placebo. Although this result is clinically significant, it is not considered astonishing. However, the discovery of GLP-1's effect on weight loss drew the attention of pharmaceutical companies (like Novo Nordisk, Eli Lily and many more) leading to extensive research and development efforts aimed at developing an improved GLP-1 peptide for effective weight-loss.
A new generation of Anti-Obesity Medications
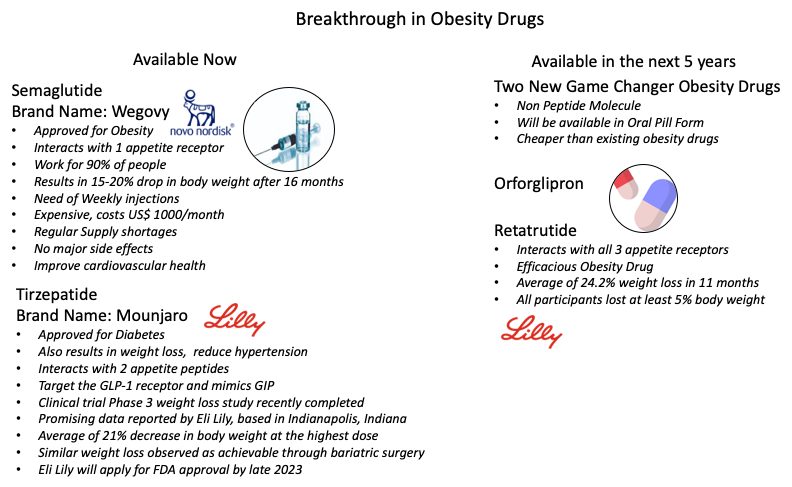
Semaglutide (Wegovy), approved in 2021, manufactured by Novo Nordisk
In early 2021, scientists were amazed by the results of a phase III clinical trial (Phase III trial provide data on a drug’s efficacy in a larger group of participants. The data collected from Phase III trials provide crucial information about the drug's effectiveness, side effects, and overall benefit-risk profile, helping regulatory authorities make informed decisions regarding its approval) investigating a new drug belonging to the same class as GLP-1 agonists: semaglutide. The trial showed that individuals who received weekly injections of semaglutide lost an average of 14.9% of their body weight after 16 months. In contrast, those who were given a placebo (inactive treatment) only lost an average of 2.4%. Importantly, no serious side effects were observed with the treatment. Moreover, individuals on semaglutide also experienced improvements in cardiovascular health, which is different from previous medications used for weight-loss.
Semaglutide is a modified version of liraglutide, the first approved anti-obesity drug. It acts on the same pathway but remains active and intact in the body for a longer duration. Additionally, it may have better access to the brain regions responsible for regulating appetite.
These results were remarkable because, historically, it has been challenging to safely achieve weight loss exceeding 10% using medication. The impressive outcomes of the clinical trial led to the FDA approving semaglutide for weight loss in adults with obesity. This approval came four years after semaglutide was first approved for the treatment of diabetes. Semaglutide is available under the brand name Wegovy and is manufactured by Novo Nordisk.
Tirzepatide, on April 27, 2023 released promising Phase 3 Trial data, developed by Eli Lily
Eli Lilly has developed a potent weight loss medication called Tirzepatide, which targets two receptors involved in glucose regulation and appetite control. This peptide drug acts on both the GLP-1 receptor and the receptor for glucose-dependent insulinotropic polypeptide (GIP), a hormone that stimulates insulin release. Under the brand name Mounjaro, Tirzepatide was initially approved for the treatment of type 2 diabetes in May 2022.
After receiving approval for diabetes treatment, Tirzepatide by Eli Lilly underwent clinical trials to assess its effectiveness in weight loss. The results of the 72-week phase 3 SURMOUNT-2 obesity trial were recently released, showcasing remarkable outcomes. Patients who were given the highest dose of Tirzepatide experienced an average weight loss of 15.7% more than those who received a placebo. Eli Lilly intends to seek approval for the drug by late 2023, which could potentially offer a new solution for weight management.
The long-term safety data for GLP-1 drugs, like Semaglutide and Tirzepatide, are encouraging. These drugs may cause mild side-effects such as vomiting, diarrhea, and nausea, but these usually improve over time.
These medications have shown great potential as highly effective weight loss treatments, bringing hope to those struggling with obesity. However, there are some barriers to access:
Daily injections are required for these drugs.
The cost of these treatments is high, around $1300 per month for FDA-approved drug Wegovy. Many insurance companies in the United States may not cover the cost due to misconceptions about obesity and considering the treatments as solely for cosmetic purposes.
Some patients may not respond well to these drugs.
While these medications offer new possibilities, it's important to address these barriers to ensure that everyone who needs them can access and benefit from them.
Breakthrough in Weight-Loss Medications: Cheaper and More Effective
The upcoming generation of weight-loss drugs aims to improve upon the effectiveness, convenience, and tolerability of the first-generation medications. This new wave includes two breakthrough drugs. The first one, called orforglipron, is easier to use and produce, and it is expected to be more affordable than current treatments. The second drug, retatrutide, has shown an unprecedented level of effectiveness, potentially setting a higher standard for treating obesity with medications.
The results from Phase II clinical trials for both drugs were recently announced at a meeting of the American Diabetes Association and published in the New England Journal of Medicine. Phase II trials provide important data on the effectiveness and optimal dosage of a drug in a smaller group of participants. These findings contribute to the ongoing development of these promising weight-loss medications.
Both orforglipron and retatrutide belong to a class of drugs known as GLP-1 agonists. However, orforglipron stands out as a non-peptide molecule that can be easily manufactured and packaged into a pill form. While its price has not been determined yet, it is expected to be much more affordable compared to existing weight-loss drugs.
On the other hand, retatrutide offers an extraordinary level of weight loss. In the clinical trial, participants who received the highest dose of retatrutide experienced an average weight loss of 24.2% over 11 months of treatment. This is higher than the typical 15-20% weight loss achieved by currently approved drugs within a similar timeframe. Retatrutide has the potential to redefine our expectations of what constitutes an effective obesity medication.
Moreover, all participants in the retatrutide study who received higher doses lost at least 5% of their body weight. In contrast, the currently approved drugs are effective in approximately 90% of individuals who take them.
These advancements indicate that orforglipron could make pharmacological weight management accessible to a broader population, while retatrutide could provide an unprecedented level of weight loss.
Resetting Expectations
The ability to achieve significant weight loss by manipulating biology supports the notion that obesity is a disease. In the past, there was a common belief among scientists and the general public that individuals with obesity were simply lacking the willpower to lose weight.
The stigma associated with obesity has hindered progress in understanding the complexity of this disease. We now know that obesity is not simply a matter of self-control but involves a complex interplay of genetic, environmental, and physiological factors. - Dr. Arya Sharma, obesity expert and founder of the Canadian Obesity Network.
Concluding Remarks
This article highlights the significant advancements in obesity medicine, offering hope for obese individuals and obese individuals with T2D who have struggled with weight loss despite making lifestyle changes. When healthy choices alone are not enough, these drugs can provide a valuable tool to shed extra pounds and avoid associated health complications. I want to emphasize that these are not medications to be used for vanity purposes.
However, it is essential to remember that maintaining a healthy and balanced lifestyle remains the foundation of a happy and thriving life. A nutritious diet, regular exercise, and sufficient sleep are crucial pillars for overall well-being.
Let us also emphasize the importance of empathy and understanding when discussing obesity. It is vital not to shame individuals for a perceived lack of willpower, as obesity is a complex condition influenced by various factors. We encourage readers to share this article with those who might benefit from its insights and support those who may be struggling with their weight.
Please Support Science Simplified!
Lastly, we kindly invite readers to consider upgrading to a paid subscription to support our newsletter. By doing so, not only will you gain access to additional benefits, but you will also contribute to the continued production of informative content that can make a positive impact on the lives of our readers.