Dear Readers,
Today we continue our explorative journey of the Endocrine System. If you have noticed, we are anatomically moving from Head-to-Toe: it started in Brain with Pineal Gland (3.2/n) than moved to neck where Thyroid gland is located (3.3/n) and now let’s explore the area between the lungs and heart where our mighty Thymus Gland is situated (3.4/n).
In this article we will examine the effects of Yoga on the Thymus Gland.
The TL;DR
Thymus gland plays a significant role in sustaining cellular immunity and long-term health. It has double duty function as an endocrine and lymphatic gland.
After puberty, the thymus starts to slowly shrink and become replaced by fat. Thymus is sensitive to stress, alcohol, smoking & drugs which can amplify the shrinkage of thymus.
Thymus shrinkage is one of the main reasons for age-related increase in cancer incidences and infections.
Yoga and Meditation can help to boost immunity indirectly by reducing stress response and directly by reducing inflammatory markers and increasing the proliferation of immune cells.
Bonus: Yoga asanas and pranayama suggested at the end of the article….
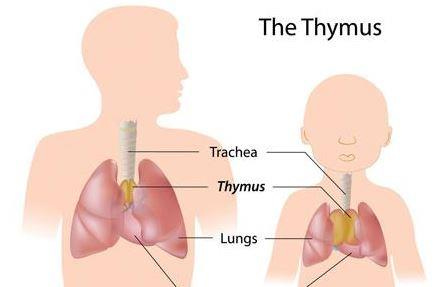
Thymus Gland anatomy in an adult (left) and in child (right)
Let’s dive deeper….
2. Thymus Gland
(According to Kundalini Yogis: Heart chakra or Anahata chakra)
The thymus is a lymphoid gland comprised of two identically sized lobes, situated in the chest behind the sternum (breastbone) and above the heart and extends upward for a short distance into the neck. It derives its name from a resemblance it bears to the bud of the thyme plant (thymus in Latin).
At puberty, it is largest in size (30-40 g) thereby in the period of adolescence the size of thymus declines (thymic involution or atrophy). In old age, it is reduced to a vestigial structure (5 g or less), the thymus epithelial cells are replaced with fat and fibrous tissue.
It is interesting to know that until 1960s the thymus was considered to be a vestigial organ with no known function. It was considered by Nobel Laureate Sir Peter Medawar “as an evolutionary accident of no very great significance” and was considered to act as a “graveyard” for dying lymphocytes (a type of white blood cells in the immune system).
The thymus was the last major organ to have its function discovered in 1961 by Jacques F.A.P. Miller. His discovery laid a foundation for immunology and modern medicine. The thymus was seen as an evolutionary relic that did little or nothing – Jacques Miller discovered it was, in fact, the conductor of the immunological orchestra. It is the mastermind organ of the immune system. Thymus has gone from the villain to the hero. Miller discovered that the thymus actually makes lymphocytes (T cells-the cellular soldiers) and sends them out into the rest of the body where they fight infections. This was the key to many other important discoveries. Now, it has also been discovered that T cells can be used to cure cancer (CAR T-cell therapy).
“He is the living person who most deserves the Nobel Prize and never got it,” declares Sir Gustav Nossal, an eminent immunologist.
“It can take many years from bench to bedside. In my case, it took nearly 60 years from the discovery of thymus function and of T and B cells to the use of T and B cells as cells that produce monoclonal antibody, and as killer cells in cancer immunotherapy”-Jacques F.A.P. Miller
2.1 Functions of Thymus Gland
Before going into the functions of thymus gland, let’s first go through simple basics about our immune system—
To survive and resist invasion by pathogenic organisms, humans have had to evolve defence mechanisms. Broadly, this defence system or our immune system can be classified as:
1. Innate or nonspecific-first line of defence against invading pathogens, relies on innate immune cells ability to recognise conserved features of pathogen and
2. Adaptive or specific-composed of specialised cells which are highly specific to particular pathogen the body has ever encountered. The adaptive immune system encompasses both
Humoral Immunity: in which antibodies are secreted as immunoglobulin molecules by B cells, and
Cellular Immunity: in which the immune response is carried out by lymphocytes (two major types of T cells: the helper T cell and the cytotoxic T cell)
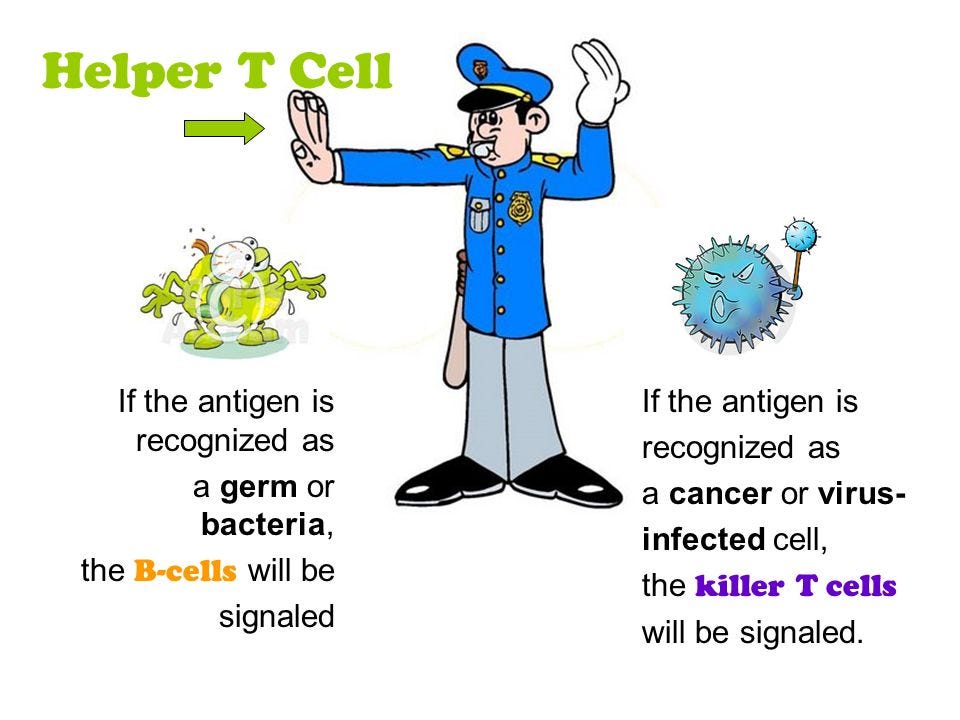
Adapted from SlidePlayer
Thymus gland plays a significant role in cell-mediated immunity and in sustaining long-term health. It has double duty function as an endocrine and lymphatic gland.
Thymus acts as :
1. Training Ground for T cells
The thymus consists of the cortex and the medulla and is divided into distinct lobules. During childhood, lymphoid stem cells that originate in the bone marrow via the bloodstream are delivered to the outer cortex of the thymus in blood. Cortex is known as the classroom of the Thymus. Here after multiplying, they then move to the inner medulla where they mature and develop T-cell surface markers. Once T cells have fully matured, they migrate to the lymph nodes throughout the body, where they aid the immune system in fighting disease.

2. Protect our body against autoimmunity
In the thymus, lymphoid progenitors commit to a specific T cell receptor and undergo positive and negative selection events that screen against self-reactivity.
In the cortex, immature T cells undergo "training," i.e. these cells are taught to recognise antigens associated with foreign cells. Cells are positively selected for usefulness.
These useful cells, that have learned to recognise specific pathogens, travel to the medulla to undergo "negative selection". In the medulla, the mature T cells are introduced to the body's own antigens. Since T cells that would react with the body's antigens could attack a person's own cells, these cells are eliminated. This prevents autoimmunity, self-attacking cells (cells that do not pass the negative selection pressure) either die or are turned into regulatory cells.
3. Hormone Production
The thymus gland produces several hormones including:
Thymopoietin and thymulin
Thymosin
Thymic humoral factor
They also produce small amounts of melatonin and insulin. Thymus epithelial cells also have receptors through which other hormones can regulate its function.
The survivors (only about 2%) of these tightly regulated positive and negative selection gates undergo complete maturation when exposed to thymus hormones, thymopoietin and thymosin. These mature T cells then leave the thymus, to form the patrolling naive T cell pool.
Thymosin also helps in stimulating growth hormone and thymic humeral factor increases the immune response of T cells in particular to viruses.
4. Thymic Macrophages
Macrophages are major population of thymus, they are distributed in an apparently random manner throughout the cortex and medulla. Macrophages are very important immune cells, known as phagocytes as they perform phagocytosis (engulfment or ingestion of dead, infected or cancerous cells-watch the video to see these amazing cells in action).
Macrophages interact with other cells in the thymus and play crucial role in T cells maturation, prevention of autoimmunity-basically they help to regulate the positive and negative selection gates.
2.2 Regulation of Thymus Gland Functions
Adult thymus functions are regulated by:
Ghrelin
Leptin
Nerve growth factor
Interleukins
These hormones and factors affect things such as food satisfaction, weight, nerve function & inflammation in our body. They are released by other glands and thus help fine tune Thymus activity.
2.3 Thymus Gland Dysfunctions
1. Immunosenesence, Inflamm-ageing: age related decline in immune system function
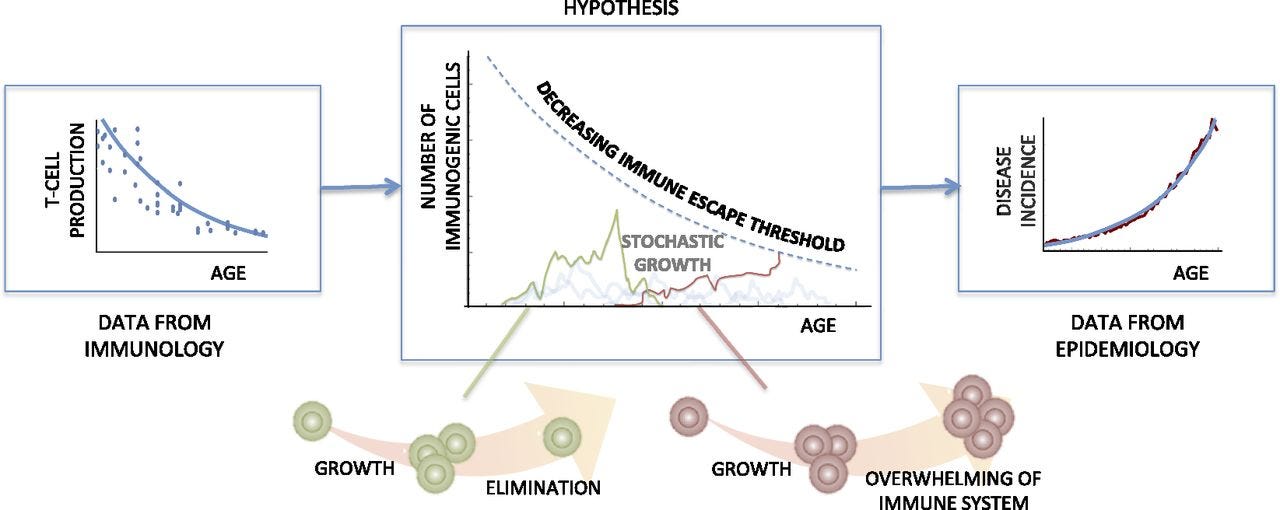
Aging is now recognised as an active process, the involution of the thymus gland may be a form of programmed aging. Decline in thymus with age leads to decrease in both T cell repertoire diversity and the proliferative capacity of naive T cells which in turn increases the risk of several infections. Accumulating evidences also suggest that immunosenescence (i.e. ageing of immune cells), rather than gradual accumulation of mutations, serves as the predominant reason for an increase in cancer incidence with age for many cancers.
Thymic involution and rising disease incidence with Age, Adapted from PNAS Article, 2017
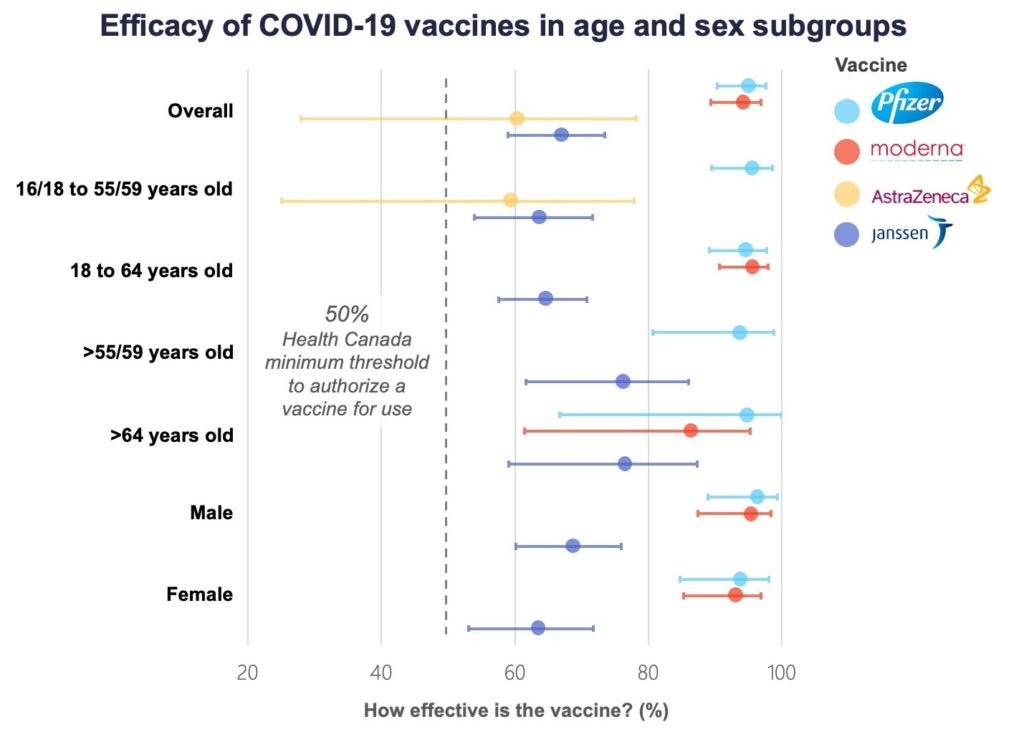
Age-associated thymic involution is also one of the reasons of reduced vaccine efficacy with ageing.
Under some circumstances, such as physiological stress, infections, malnutrition and pregnancy, thymus can undergo transient or reversible thymic decline. The thymus is also sensitive to alcohol, cigarettes and drugs of any type. Sometimes, this happens due to state of oxidative imbalance characterised by a greater number of pro-oxidants than anti-oxidants. This situation is quite detrimental to thymus function.
The antioxidant nutrients most important for protecting the thymus include the carotenes, vitamin C, vitamin E, zinc, and selenium. Early studies suggest that calorie restriction may slow the atrophy, but the research is still in its infancy.
2. Hyperplasia of the Thymus
Overactive thymus gland (i.e. Hyperplasia)-most often it occurs in autoimmune disorders such as Myasthenia Gravis (associated with muscle weakness in the voluntary or skeletal muscles of the body), Graves' disease, and Lupus. The clinical symptoms of hyperactive thymus are pale skin, lymphatic node hyperplasia, tonsillitis and rhinitis.
3. Hypoplasia/Aplasia of the Thymus
DiGeorge syndrome is developmental disorder, caused by a gene mutation. It is an uncommon condition marked by a significant reduction (i.e. Hypoplasia) or absence (i.e. Aplasia) of thymus function, children with this condition have severe immunodeficiency and a high risk of infections. Another congenital disease is severe combined immunodeficiency–a genetic disease involving a lack of both T and B lymphocytes. In such cases the thymus gradually disappears.
4. Thymomas
Thymomas are tumors in the epithelial cells of the thymus. Thymomas may also cause a condition referred to as thymoma-associated multiorgan autoimmunity. Overall, tumors of the thymus are rare.
2.4 Can Yoga help to balance Thymus Gland?
Scientific Evidences:
Accumulating evidences from 15 randomised controlled trials revealed a general pattern suggesting that yoga can down-regulate pro-inflammatory markers, like interleukin-1-beta, interleukin-6 and Tumor Necrosis Factor-alpha. These findings indicate that yoga may be implemented as a complementary intervention for populations at risk or already suffering from diseases with an inflammatory component.
Another study carried out on n=60 first-year MBBS students randomly assigned to yoga group and control group. The yoga group underwent integrated yoga practices for 35 min daily in the presence of trained yoga teacher for 12 weeks. Control group did not undergo any kind of yoga practice or stress management. Findings demonstrated decrease in serum IFN-γ levels with examination stress (brief naturalistic stressors). Decreased serum IFNγ levels indicate decline in cellular immunity. In Yoga group, the decrease in serum IFNγ was less significant compared with that in the control group. Study concluded that even 12-week of yoga intervention can help in balancing immune response in face of stressful situation.
Research done in patients suffering from pulmonary tuberculosis demonstrated that 2 months of yoga practice can potentiate the body’s immunity and action of antitubercular drugs. Researchers observed significant reduction in symptom scores and an increase in weight, pulmonary functions. This study suggest a complementary role for yoga in the management of pulmonary tuberculosis.
Yoga and Meditation practice has been scientifically evidenced (in detail these scientific studies have been discussed in articles 1/n & 2/n) to reduce stress levels by activating the parasympathetic nervous system (vagus nerve stimulation, rest response) and deactivating sympathetic nervous system (flight-and-fight response). Also in earlier articles we have discussed in great detail about the effects of long-term meditation practice on reduction in amygdala functions (stress centre in Brain), brain waves. There is strong evidence of stress playing a major role in suppressing immune responses and also it amplifies the process of thymus involution.
It is thus logical to conclude that effects of Yoga and Meditation on Thymus Gland are mostly indirect.
Another interesting study suggested that 10-week group-based cognitive behavioural stress management (CBSM) intervention on HIV patients (severely suppressed immune functions) resulted in decrease in 24-h urinary cortisol (with reduced depressed mood) and norepinephrine (with reduced anxiety) and increases in serum DHEA-S and testosterone levels (with reduced depressed mood). This study also found increase in immune cells indicating boost in immune functions post CBSM program. In conclusion this study is promising, however many more such studies are required to understand the mechanisms of Yoga and Meditation intervention on immune functions.
Overall, this field of investigation is still young, hence the current body of evidence is small and for most immune parameters, more research is required to draw distinct conclusions.
Yoga asanas, Meditation and Breath Work to balance dysfunctional thymus gland symptoms (list is not exhaustive):
Dhanurasana or Wheel Pose
Bhujangasana or Cobra Pose
Matsyasana or Fish Pose
Kurmasana or Tortoise pose
Adho Mukha Svanasana or Downward Facing Dog pose
Bhramari Pranayama or The Humming Bee Breathing Technique
Kapalbhati Pranayama or Forehead Shining Breathing Technique
Anuloma Viloma Pranayama or Alternate Nostril Breathing Technique
Bhastrika Pranayama or Bellow Breathing Technique – Breath of Fire
If you found the article of interest or have thoughts about what you’ve read here, please do share in the comments section below. It will help guide my future posts.
In the next article (3.5/n), I will cover the science behind the effects of Yoga on the Adrenal glands. Until then, Stay healthy and happy :)
Knowledge is power. It grows with sharing….Share Dr-Yoga’s free weekly newsletter with someone who enjoys reading and curious to dig deeper into the topics you care about most.