Dear Readers,
Welcome to Science Simplified, a newsletter which Unlocks the Wonders of Science, One Simplified Concept at a Time!
This post will break down the basics of mRNA vaccine. While the term ‘mRNA vaccine’ has become increasingly common over the past two years, many people still lack a completely understanding of how it works, its distinctions from traditional vaccine manufacturing methods, whether it makes permanent changes in genome, how these vaccines can be rapidly developed, their thorough testing, potential long-term effects, and various related queries. This post intends to demystify some of these mysteries surrounding the use of mRNA in immunisation. We’ll delve into comparing this new approach with the conventional vaccine manufacturing methods and briefly describe how mRNA vaccine work inside your bodies.
mRNA is likely to be at least one of the waves of the future for vaccines- Ingrid Scully, PhD, Senior Director of Vaccine Research and Development at Pfizer
In the subsequent post, we’ll specifically address the adverse side-effects associated with COVID mRNA vaccines. To stay updated and support my work, consider becoming for new posts, both free or paid options available.
Science Simplified, is a reader-supported publication that covers diverse topics directly impacting your lives. Your support in any which way is greatly appreciated.
1. Let’s begin with Basics!
1.1 What is mRNA?
mRNA stands for messenger RNA (Ribonucleic Acid). True to its name, mRNA acts as a messenger by carrying the encoded messages from DNA (the human genetic code) to ribosomes. Ribosomes then interpret these messages to create proteins, which serve as the functional building blocks in our bodies. mRNA is single-stranded and consists of four base pairs: A, U (T), G, and C, which complement the DNA codes. Unlike DNA, mRNA is not stable and gets degraded by biological mechanisms once the protein message is translated. Proteins play diverse roles within our bodies: they can act as structural components for skin, bones, muscles, hair, and nails; they function as carriers, enzymes, hormones, neurotransmitters, and are essential components of the immune system like antibodies.

Think of mRNA as a messenger in your body. It carries important instructions from the genetic code (DNA) to the places that make proteins. These proteins are like workers in your body, doing lots of different jobs. Once mRNA delivers its message and the protein is made, it's like the messenger gets 'snipped' or cleaned up, as its job is done.
1.2 What are Vaccines?
Vaccines act os trainers for our immune system. Our body's defense system is smart—it can identify and fight off invaders like viruses or bacteria. But the first encounter with a new invader can be slow and risky.
This slow response can strain the body and lead to serious consequences, particularly when the immune system is weakened due to underlying health conditions, aging, pregnancies, or in the case of children with still-developing immune systems. Moreover, if the invader is new and has the potential to evade the immune system, like many viruses and some bacteria can do, our immune system requires assistance. Vaccines step in to help.
They train the immune system, teach them to recognise and combat specific invaders without causing you to get sick from the actual infection. It is like giving the immune system a heads-up, so if the real invader shows up, our body can respond faster and stronger preventing us from becoming seriously ill.
2. Conventional versus mRNA Vaccines
2.1 Pioneering history of Vaccines
Vaccines are not a new concept; they have been around for a considerable time. The first vaccine in history is attributed to Edward Jenner in 1796. Jenner's work with the smallpox vaccine paved the way for the eventual eradication of this highly contagious and deadly disease caused by the variola virus. The global eradication of smallpox was officially declared on May 8, 1980, marking one of the most significant achievements in public health history.
Since the development of the first vaccine, we have expanded our arsenal to include multiple vaccines that have saved billions of lives from various deadly and contagious pathogens. While smallpox has been successfully eradicated, efforts continue to eliminate other contagious and dangerous preventable diseases like polio, measles, rubella, and mumps globally.
If interested to learn more about the history of vaccination: click here.
2.2 Lessons learned from the First Successful Vaccine
The first vaccine originated from material taken from a cowpox sore on a milkmaid’s hand. Edward Jenner introduced the material into a healthy boy named James Phipps, which made him immune to smallpox. Since then the field of vaccines has evolved significantly. Today, vaccine manufacturing processes undergo stringent regulation, rigorous quality control and extensive clinical testing before being administered to individuals.

To grasp the advancements, it’s essential to comprehend why Edward Jenner’s vaccine was successful. His success with the rudimentary approach was grounded in a profound observation and a fundamental understanding of how the immune system functions. He observed that individuals infected with cowpox, a mild-relative of smallpox, seemed to be cross-protected to smallpox. Additionally, by deliberately introducing cowpox material, a weakened form of pathogen conferred immunity without causing illness to a healthy individual. This concept laid the groundwork for the development of vaccines against various diseases.
2.3 Vaccine Manufacturing Methods
Currently, we have six different ways to develop a vaccine. Moreover, there have been advancements in the ways vaccines are administered—from needle injections and nasal sprays to oral doses, a more recent innovation.
1. Live-attenuated vaccines
Live-attenuated vaccines contain live pathogens from either a bacteria or a virus that have been "attenuated," or weakened. This means that the weakened pathogen can still produce a robust enough immune response but that does not cause disease. Additional booster dose is not needed with live-attenuated type vaccine.
Examples: Measles, mumps, and rubella (MMR) vaccine, varicella (chickenpox) vaccine
2. Inactivated vaccines
Inactivated vaccines take a live pathogen and inactivate or kill it. The inactivated pathogen is strong enough to create an immune response, however, is incapable of causing disease. The immune response is not as strong as live-attenuated vaccine and hence multiple doses are often needed in order to build up immunity and offer full protection.
Examples: Polio and Influenza vaccine
3. Subunit vaccines
Subunit vaccines are made from a piece of a pathogen, not the whole organism, so they do not contain any live pathogens. They are suitable for older people, children and immunocompromised individuals.
Examples: Haemophilus influenzae type B (Hib) vaccine (conjugate), pneumococcal vaccine (polysaccharide or conjugate), shingles vaccine (recombinant protein), hepatitis B (recombinant protein), acellular pertussis, MenACWY (conjugate).
4. Toxoid vaccines
Toxoid vaccines use inactivated toxins to target the toxic activity created by the bacteria, rather than targeting the bacteria itself. Booster shots are typically recommended every 10 years or so.
Examples: Tetanus vaccine, diphtheria vaccine
5. Viral Vector vaccines
Viral vector vaccines use a harmless virus to deliver to the hosts cells the genetic code of the antigen you want the immune system to fight. In doing so, information about the antigen is delivered, which triggers the body’s immune response.
Viral vector vaccines usually trigger a strong immune response. Typically, only one dose of the shot is needed to develop immunity. Boosters may be needed to maintain immunity.
Examples: Ebola vaccine, COVID-19 vaccine (AstraZeneca and Johnson & Johnson)
6. mRNA Vaccines
The mRNA vaccine carries the RNA material, once administered they teaches our body how to make a specific type of protein that is unique to the virus, but does not make the person sick. The protein triggers an immune response, which includes the generation of antibodies that recognize the protein. That way, if a person is ever exposed to that virus in the future, the body would have the tools (antibodies) to fight against it.
Examples: Pfizer-BioNTech COVID-19 vaccine (Comirnaty®), Moderna COVID Vaccine (Spikevax®).

At their core, all vaccine manufacturing techniques share a common goal: priming our immune system to anticipate and combat future infections. Think of vaccines as preemptive 'ID cards' showcasing the most-wanted pathogens to our defense cells. These 'IDs' come in various forms—live-weakened, inactivated, fragments of the pathogen, its toxin, a vector delivering the pathogen's message, or even mRNA carrying instructions for producing a specific protein from the pathogen.
By presenting this advance information, vaccines empower our immune 'army' to recognize, prepare, and swiftly neutralize these threats, should they ever invade our system. Each type of vaccine acts as a strategic training manual, helping our body gear up for potential encounters with specific diseases.
2.4 Difference between Conventional and mRNA Vaccines
Conventional vaccine manufacturing techniques and mRNA vaccines diverge significantly in their approaches to immunization:
Manufacturing Speed and Scalability: Conventional vaccines requires specialised facilities and processes for culturing, inactivation and formulation. mRNA vaccines on other hand represent groundbreaking leap, their development process is faster and more adaptable. They utilize the body's cellular machinery to produce a targeted immune response, offering potential advantages in speed of production, scalability, and versatility.
Response Time and Adaptability: Conventional vaccines often require longer development timelines due to the need for pathogen cultivation, inactivation, and purification processes. In contrast, mRNA vaccines can be rapidly designed once the genetic sequence of the pathogen is known, offering a quicker response to emerging threats. This adaptability proved crucial during the COVID-19 pandemic, allowing for the swift development of mRNA-based COVID-19 vaccines.
Stability and Storage: Conventional vaccines often necessitate specific storage conditions, such as refrigeration or freezing, to maintain stability. mRNA vaccines, although initially sensitive to temperature fluctuations, are generally more stable and may offer advantages in terms of distribution and storage once optimized.
3. Decades in making mRNA act like a vaccine
Decades were spent making mRNA function like a vaccine. Discovered in the early 1960s, mRNA held therapeutic promise, yet its transient nature posed a challenge. Over the years, hundreds of scientists worked tirelessly, refining methods and innovating technologies to effectively harness mRNA as a vaccine. The COVID-19 pandemic hastened research already underway for decades.
The major challenges to use mRNA effectively as a therapeutic agent or vaccine was to ensure its successful entry into cells, protecting it from degradation, and facilitating efficient translation into proteins without triggering the body’s inflammatory response.
The solution came from groundbreaking work of scientists Katalin Karikó and Drew Weissman, who focussed on nucleoside base modifications. Their work proved pivotal in developing highly effective mRNA vaccines against COVID-19. Their pioneering research addressed critical challenges by enhancing mRNA stability, reducing its susceptibility to degradation, and minimizing its potential to trigger unwanted immune responses.
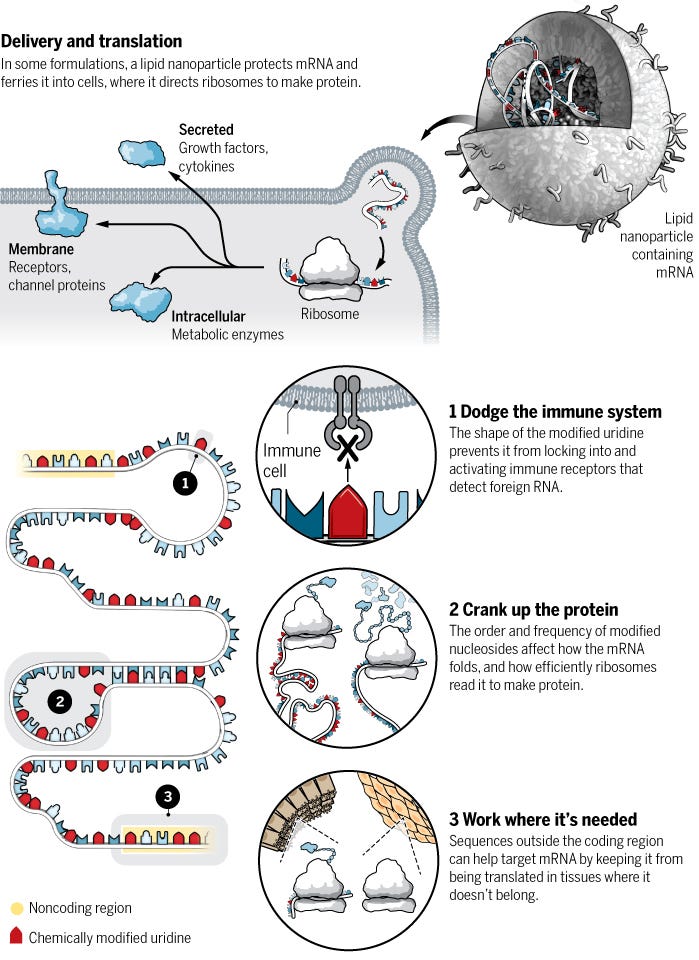
Furthermore, advances in nanotechnology offered a solution: the development of fatty droplets (lipid nanoparticles) that wrapped the mRNA like a bubble, enabling its entry into the cells. Once inside the cell, the mRNA message could be translated into proteins, such as the spike protein of SARS-CoV-2, and the immune system would then be primed to recognize the foreign protein.
In recognition of their monumental contributions, Katalin Karikó and Drew Weissman were jointly awarded the Nobel Prize in Physiology or Medicine in 2023, celebrating their remarkable achievements in revolutionizing mRNA technology. For a deeper dive into their inspiring journeys leading to this groundbreaking discovery, explore the earlier article in Science Simplified.
The COVID-19 mRNA vaccines were created in record time for three main reasons: First, scientists already knew a lot about similar viruses. Second, they'd been studying mRNA for years. And third, they sped up the usual vaccine-making process.
The virus causing COVID-19 belongs to a family of viruses we've seen before. Scientists had a head start because they'd studied these viruses for a long time. Using this knowledge, they quickly used a cool technology called mRNA to make potential vaccines.
Lots of countries and researchers worked together and got lots of money to run tests at the same time. This helped speed things up. Luckily, their risky plan worked better than expected. Not only did they make a COVID-19 vaccine, but they also showed how teamwork and faster ways of doing things in science can solve big health problems.
Want to know more, read The History of mRNA Vaccine Applications.
4. Will mRNA vaccine make permanent changes to genome?
No, they will not. Due to mRNA's nature, it does not enter the cell nucleus, where DNA resides, nor does it interact with or modify the DNA sequence. Consequently, it lacks the ability to cause permanent changes or mutations to the genome. The mRNA used in these vaccines is temporary and does not become part of the cell's genetic material. Therefore, mRNA vaccines are considered safe, as they do not alter an individual's genetic makeup.
mRNA functions as a transient messenger, providing instructions to the cell's protein-making machinery before being degraded or removed.
Additionally, concerns about mRNA converting into DNA and integrating into the genome are unfounded in the case of COVID-19 mRNA vaccines. The enzyme required to convert mRNA to DNA is absent in both humans and coronaviruses. In essence, mRNA vaccines cannot induce permanent changes in DNA (genome).
5. Conclusion
Harnessing the power of mRNA for vaccines marks a new era in vaccine technology and production, showcasing the incredible progress achieved through decades of scientific research. It's a testament to our evolving understanding and application of science in addressing global health challenges.
Hope this article clarified some of the mysteries about mRNA vaccines. Should you have any queries about mRNA COVID-19 vaccines or this technology in general, please feel free to ask.
Stay tuned for our upcoming article, which will delve into potential side effects of COVID-19 mRNA vaccines. Subscribe to our newsletter for direct access to new posts and the opportunity to ask questions.